Exercise and Blood Pressure
Like most other chronic diseases and risk factors, exercise is highly effective for both preventing and treating high blood pressure. Almost all types of exercise have some effect. Some are more effective than others, and some are more effective than you might think.
Here’s my Youtube video on this same subject if you prefer to watch than read:
Before we begin, it’s important to have a basic understanding of what blood pressure is, what constitutes normal blood pressure, and how blood pressure responds both acutely and chronically to exercise.
What is Blood Pressure?
Blood pressure is a measure of how much pressure there is in your circulatory system. The circulatory system is complex. For our purposes in this article, you can think of it as a system of tubes, your arteries and veins, and a pump, your heart.
There are two numbers in a measure of blood pressure. The first number, called systolic, is the pressure on the system when the heart pumps, and the second number, called diastolic pressure, is the pressure on the system when the heart relaxes. The higher the number, the more pressure on the system. The more pressure on the system, the harder the heart is working.
Because the first number is the pressure on the system when the heart is actively pumping, this number is always higher than the second number, and it can go much higher safely, during exercise. Because the second number is the pressure during relaxation on the system, it doesn’t go quite so high, and it’s more problematic if that number becomes chronically elevated.
What is Healthy or Normal Blood Pressure?
This is important to understand because “normal” or healthy blood pressure during rest and during exercise are very different. If you’re doing a hard workout, your heart is working hard, and your blood pressure will be elevated. In a healthy person, this is completely fine. If you’re relaxing on the couch and your blood pressure is elevated, that’s when problems can occur. If the heart is working hard when it should be resting, it becomes overtaxed and heart disease develops.
The main process through which blood pressure gets higher over time is a gradual hardening of the arteries. Lack of exercise aggravates this. When we work hard during exercise, the pumping of the heart makes the blood vessels expand and contract. Just like lifting weights stimulates your muscles and keeps them healthy, it can also stimulate your arteries and veins to keep them healthy.
When it comes to “normal” or “healthy” blood pressure, the numbers most people are familiar with are 120/80, but the guidelines were actually revised a few years ago now so that 120/80 rather than being healthy or perfect, is the upper limit of healthy or normal blood pressure.
It’s quite common in healthy people to have resting blood pressure quite a bit lower than 120/80. Low blood pressure like this is not necessarily a problem, only if it doesn’t rise to meet the intensity of the task.
This image provides a summary of the current classifications for healthy and elevated blood pressure.
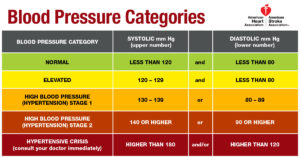

You can see that resting systolic blood pressure slightly above 120 is considered elevated, 130-139/80-89 is considered Stage one hypertension, and 140/90 or more is Stage two hypertension.
Blood Pressure Response to Exercise
What is healthy and normal for a blood pressure response to exercise is completely different than blood pressure during rest. Elevations in blood pressure in response to exercise are completely normal and expected.
The amount which blood pressure increases will depend on the person and the activity. In a healthy young person, we don’t need to be concerned about blood pressure rising in response to exercise. MacDougall and colleagues measured a mean reading of 320/250 and as high as 480/350 in trained body builders during a leg press exercise, with no adverse effects.
It’s critical that I mention that these readings and findings relate to young, healthy people with “normal” blood pressure. For people who have or think they may have high resting blood pressure or other risk factors, it’s critical to speak with your doctor or work with a qualified exercise professional before changing or increasing your physical activity or exercise levels.
It’s also important to understand that when properly facilitated and with appropriate consultation from medical and other health professionals, that the risks of exercise are much less than the risks of not exercising.
Researchers, regulatory bodies like the American Heart Association, American College of Sports Medicine, Canadian Society for Exercise Physiology all agree that exercise is a cornerstone therapy for the prevention, treatment and control of hypertension.
Any type of exercise can have a beneficial effect on blood pressure and other measures of cardiovascular health. Aerobic activity is the most effective, but strength training and stretching can be effective too.
Getting Active with High Blood Pressure
For someone who is not currently exercising, the best place to start would be to start working up towards the minimum physical activity guidelines for walking: 30 minutes of walking per day, 5 days per week, accumulated in bouts of 10 minutes or more. Once someone reaches this activity threshold, we can then look at increasing time, intensity, or add in new types of activity that make sense for the person. In the case of blood pressure, increasing frequency and exercise time should be prioritized over intensity. These variables provide additional benefit and likely not pose any additional risk. In contrast, intensity, although valuable and should be pursued at some point, does increase the risk of adverse events for higher risk people.
Although aerobic exercise is the best way to keep blood pressure healthy and to control blood pressure for a person with higher blood pressure, resistance training or strength training can also play an important role.
Resistance Training and Blood Pressure
Cornelissen and colleagues performed a meta-analysis on randomized control trials that investigated the effect of resistance training on blood pressure and found that it although it reduced blood pressure in both normotensive and hypertensive groups, that the reduction in the hypertensive groups was not significant.
However, the authors importantly noted that the strength training interventions consistently and significantly improved other important measures of health and fitness like VO2 max, body composition, blood lipid profile and more.
Something that is important to consider when talking about exercise for the management of chronic disease is that we can’t look at risk factors in isolation. Blood pressure is one of many components of cardiovascular health, and these components are all connected. People with elevated blood pressure will often have other risk factors like increased waist circumference, or elevated triglycerides. Exercise programs work best when they address the whole person.
Although aerobic exercise is more effective for controlling blood pressure, resistance training can be safe, and can help improve blood pressure through other mechanisms, even if we don’t fully understand them.
Designing a Training Program for Managing Blood Pressure
There aren’t established guidelines for the exact best resistance training protocol for targeting blood pressure. We can start with general guidelines and then modify based on common sense and available research.
Stewart and colleagues conducted a randomized control trial investigating the effect of RT on adults aged 55-75 with mild, untreated hypertension. The study participants followed a fairly standard program. They completed three supervised exercise sessions per week that included a warmup, strength training and aerobic training – pretty standard. The strength training protocol was 2×10-15 reps at 50% of predicted 1RM. I thought this was interesting. In a healthy or low risk population, you would typically prescribe an intensity of 70% 1RM for that rep zone. Lowering intensity in this way is is a good strategy for limiting excess afterload on the heart, which needs to be managed in higher risk populations.
A person doing strength training as part of a plan to manage blood pressure would do well to follow similar frequency and exercise selection as a lower risk person. Reducing intensity is an effective modification specific to managing high blood pressure.
Exercise and Blood Pressure: Summary
An important takeaway from the research on strength training and blood pressure is that strength training does not chronically elevate blood pressure. Although an acute bout of exercise does elevate blood pressure, this is temporary. And the benefits of strength training, which include but go well beyond controlling blood pressure, outweigh the risks.
There is another way to think about this. Often times the absence of exercise is a major contributing factor to the development of hypertension in the first place. It’s logical that adding exercise would help resolve the situation, as well as providing an array of indispensable health benefits.
If you are interested in becoming more active to help manage your blood pressure, that’s awesome. Working with your doctor or a qualified exercise professional is the best place to start. But also, do not be afraid to become more active. The benefits of exercise far outweigh the risks, and the risks of not exercising are very real.
If you’re interested in personalized guidance and help with increasing your physical activity levels, get in touch to find out if our online coaching or personal training services are right for you!
Want Strong Abs?
Get Core Strength Essentials
blood pressure, exercise, exercise for blood pressure, exercise for hypertension, fitness, health, hypertension

Dave
Great fact supported presentation.
Thank you!